What is a Bloodless Scalpel?
Under the shadowless lights of the operating room, a surgical procedure is underway. Unlike traditional surgical scenes, there are no frequently replaced metal scalpels, no noticeable burning smell, and minimal bleeding. The surgeon’s instruments seem to perform the cutting and hemostasis quietly. All of this is thanks to a revolutionary surgical tool—the ultrasonic scalpel.
What is an ultrasonic scalpel?
An ultrasonic scalpel, also known as an “ultrasonic cutting and hemostatic scalpel,” is a surgical instrument that uses high-frequency ultrasonic energy to cut and coagulate soft tissue. It is not a “scalpel” in the traditional sense, but rather an energy platform that converts electrical energy into mechanical vibration to enable precise, minimally invasive surgical procedures.
The key to the ultrasonic scalpel lies in its tip—a metal blade that vibrates at a frequency of 55,500 times per second. This frequency far exceeds the upper limit of human hearing (approximately 20,000 Hz), which is why it is called “ultrasonic.”
How does an ultrasonic scalpel work? How is vibration converted into cutting force?
- The Energy Conversion Process
The operation of an ultrasonic scalpel begins with a precise energy conversion process:
The main unit converts ordinary electrical energy into a high-frequency (55.5 kHz) electrical signal.
A piezoelectric ceramic element inside the scalpel’s handle receives this signal and generates tiny but high-speed mechanical vibrations.
This vibration is amplified by a set of “amplifier rods” mechanical devices.
Ultimately, the vibration amplitude at the tip of the scalpel reaches 50–100 micrometers—thinner than a human hair, yet extremely fast.

- The Triple Effect on Tissue
When the vibrating scalpel head comes into contact with tissue, three mechanisms act simultaneously:
Mechanical Effect: Tens of thousands of vibrations per second directly disrupt cell structures, causing the tissue to be torn apart with minimal force. Each tear is extremely small, ensuring precise cutting.
Thermal Effect (the key): Under intense vibration, protein molecules within the tissue rub against each other, generating heat. This heat is “endogenous” and not external. When the local temperature reaches 60–100°C, the proteins denature and coagulate, and blood vessels constrict.
Cavitation Effect: High-frequency vibrations create countless tiny bubbles in the tissue fluid, which burst instantly, helping to separate tissue layers and making the cut cleaner.
Notably, the heat generated by the ultrasonic scalpel is confined strictly to the area where the instrument touches the tissue—typically affecting only 0.5–1 mm. In contrast, the heat spread of a traditional electroscalpel can reach 3–5 mm. This precise thermal control is the foundation of modern minimally invasive surgery.
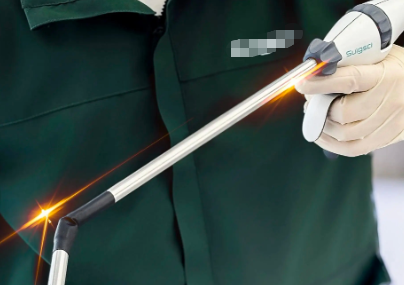
Why is it superior to traditional tools? Five major advantages of the ultrasonic scalpel:
- Simultaneous cutting and hemostasis
This is the most significant advantage of the ultrasonic scalpel. In traditional surgery, cutting (with a scalpel) and hemostasis (using electrosurgery or ligation) are separate steps. The ultrasonic scalpel combines these two functions, especially for blood vessels smaller than 3 mm, allowing for immediate closure. This significantly reduces bleeding and shortens the surgical procedure.
- Reduced thermal damage and smoke
Compared to the high temperatures of 300-400°C generated by electroscalpels, ultrasonic scalpels typically operate at temperatures below 100°C. This results in less thermal damage to surrounding tissues. Additionally, they do not produce electrical sparks, reducing smoke by approximately 70%. This ensures a clearer surgical field and lowers the risk of medical staff inhaling harmful fumes.
- Avoids current passing through the patient’s body
Traditional electrosurgical devices require electricity to pass through the patient’s body, which poses a risk of burns. Ultrasonic scalpels rely on mechanical vibrations, eliminating the need for electric current. This makes them safer, especially for patients with pacemakers.
- Precise Layered Separation Capability
The vibrational properties of ultrasonic scalpels enable more precise separation of tissues along their natural layers. This provides better protection for vital structures such as nerves and blood vessels and makes it easier to identify them during surgery.
- Multifunctional Integration
One device can perform multiple operations, including grasping, separating, cutting, and coagulating, thereby reducing the need for instrument changes and improving surgical efficiency.
Clinical Applications: Changing the Surgical Landscape
Originally used in laparoscopic surgery, the ultrasonic scalpel has now become widely applicable in nearly all surgical fields:
General Surgery: Protecting the recurrent laryngeal nerve during thyroid surgery; managing blood vessels during gastrointestinal procedures.
Gynecology: Hysterectomy, myomectomy, reducing bleeding, and protecting ovarian function.
Urology: Prostatectomy, partial nephrectomy.
Thoracic Surgery: Managing blood vessels and bronchi during lobectomy.
For example, in thyroid surgery, traditional methods may result in 50–100 ml of blood loss, whereas the use of an ultrasonic scalpel can reduce this to less than 10 ml, thereby shortening operation time by 30% and significantly accelerating patient recovery.
Limitations: No tool is perfect.
The ultrasonic scalpel is not a panacea:
Its effectiveness is limited when it comes to closing larger blood vessels (>5mm in diameter).
Overuse or improper application can still cause thermal damage.
The equipment is expensive, and the scalpel blade is designed for single-use only.
Specialized training is required to make the most of its effectiveness.
Future prospects: Smarter energy-based surgical techniques
Next-generation ultrasonic scalpels are becoming more intelligent:
Real-time feedback systems monitor tissue impedance and automatically adjust energy output.
More precise frequency control allows different vibration settings for various tissue types.
Nano-scale scalpel blades enable ultra-precise manipulation at the cellular level.
Robotic integration: Deep integration with surgical robots for unmanned, precise operations.
Since its FDA approval in early 2000, the ultrasonic scalpel has transformed from a “novel tool” into a “surgical standard.” More than 5 million surgeries worldwide use ultrasonic scalpel technology annually.
Click to return to the home page
[…] Understanding the principles of ultrasonic scalpel […]